AR Recovery Services
Medcod offers a comprehensive range of AR management services, recovering outstanding revenue from old AR accounts that are aging more than 120 days. Our system has been proven to be highly effective at increasing recovery, even from accounts that were thought to be lost causes.
Unlike most medical billing companies, who only offer AR recovery solutions as part of a revenue cycle management package, MedCare MSO offers AR medical billing recovery services as a standalone option. We don’t believe in a one-size-fits-all approach to healthcare receivable recovery services and want to meet the unique needs of your business.
Case Study Results

1st April
Started On

1 Year
Review Period

$86,000 to $144,000
Collection Increased

67 %
Revenue Increased By
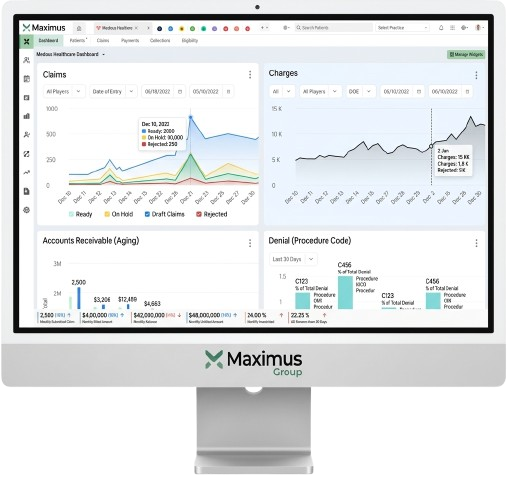
Systematically increasing revenue with effective claims management
Medcod innovative system tracks every claim to completion, getting our clients the revenue they deserve.
MedCod 4-Part Strategy for AR Recovery
Our strategy for managing aging AR accounts has been developed through years of experience. Our old AR recovery service is a streamlined approach that is both fast and effective.

Systematic Evaluation
When our AR team offers account recovery solutions to a new client, the first step is a thorough review of every unresolved claim. There may be some that have expired or are not collectable for some other reason, but we find every one that can possibly be recovered and get to work on it. We aren’t just looking for the “low hanging fruit” in this process. Many HIPAA-compliant billing companies only look for high dollar claims in aging AR, but we know how fast the smaller amounts add up for our clients, so we look at any claim that could still be paid.
Prioritization
Our team analyzes older unpaid claims as a high priority to ensure that none expire before we get a chance to process them. Using advanced analytical tools to minimize medical account receivables, we stay ahead of the payers’ requirements to help you collect the maximum revenue possible. We consistently follow up with each payer to recover your overdue payments so you can focus on your practice, knowing that we are looking after your bottom line.
Claim Correction and Resubmission
Our dedicated taskforce doesn’t let a single claim be rejected, denied or underpaid due to lack of follow-up. After the appropriate corrections or clarifications are made, we appeal each of those claims so the insurance or government payer will reconsider the payment. We also monitor your claim denials and rejections, so we can identify any recurring causes and eliminate them permanently from your revenue cycle management system.
Patient Communication
If the AR team finds that the outstanding balance should be paid by the patient, we generate a report that is easy for them to understand and send it to them. If you would like us to also handle the direct interactions with your patients, we will do that too. We aren’t a collection agency, so you don’t have to worry about sending the wrong message to your patients. We’ve found patients are much more likely to pay their bills if they understand the charges and agree with the amount due, so we help make everything clear and easy to understand. We’ll even take their phone calls and answer questions if you would like us to.

AR Recovery Is One of Our Specialties
A tremendous amount of revenue is lost every year due to unpaid claims not being managed properly. We have a dedicated AR recovery team that is extremely successful at getting reimbursements for what others consider “uncollectible.” It is well known in the collections industry that the longer a bill goes unpaid, the less likely it is to be paid—but rather than giving up on old AR recovery & bills. Our account Receivable recovery services team takes that as our cue to take immediate action towards identifying and investigating every unpaid claim. Few medical AR billing services are willing to take on aging AR, or if they do, they want a high fee. Our system streamlines the process, allowing us to be efficient enough to work profitably on old AR Recoveries and low-value claims. These are some of the features of our AR recovery system.
Payment Posting
We post payments, adjustments, and denials in real time to ensure accurate reconciliation and faster revenue processing with minimized billing errors.
Medical Coding
Accurate CPT, ICD-10, and HCPCS coding to maximize reimbursements while ensuring compliance with insurance regulations.
Claims Submission
Fast and clean claim submissions to reduce rejections and speed up insurance approvals for better cash flow.
Eligibility Verification
Verify patient insurance eligibility before appointments to reduce claim denials and improve efficiency.
AR Management
Proactive accounts receivable follow-ups to minimize outstanding balances and improve revenue cycle performance.
Denial Management
Identify root causes of denials, resubmit corrected claims, and reduce future claim rejections effectively.
Charge Entry
Accurate charge entry from superbills to prevent revenue leakage and maintain clean billing records.
Revenue Reporting
Detailed financial and performance reports to help practices track revenue growth and optimize billing strategies.








