Chronic & Principle Care Management
Our PCM and CCM solutions enable providers to deliver continuous care beyond office visits while maximizing reimbursement. We ensure accurate, compliant coding, patient eligibility management, and coordinated care, while reducing denials through AI-powered pre-billing validation and end-to-end revenue cycle management, keeping patients engaged and practices properly reimbursed.
Case Study Results

Collection Ratio
96 %

Trusted by
100 + Providers

Revenue Increased
35 %

Serving Specialties
50 %

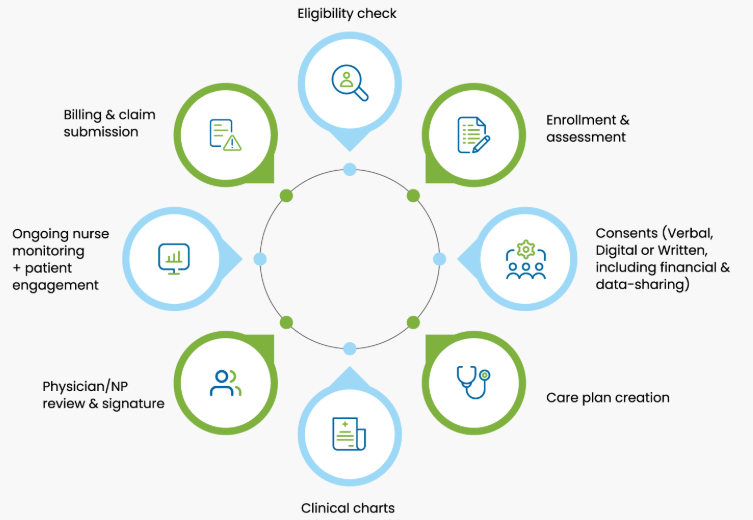
Principle Care Management Solutions & Documentation Support
Strong principle care management solutions are central to effective PCM programs. Our PCM solutions validate care plans, care coordination notes, and non-face-to-face clinical activities. We ensure documentation clearly supports the time spent managing chronic conditions. This allows providers to focus on patient outcomes while maintaining clean, compliant records that fully support principle care management billing.
Principle Care Management Solutions & Documentation Support
Strong principle care management solutions are central to effective PCM programs. Our PCM solutions validate care plans, care coordination notes, and non-face-to-face clinical activities. We ensure documentation clearly supports the time spent managing chronic conditions. This allows providers to focus on patient outcomes while maintaining clean, compliant records that fully support principle care management billing.


Chronic Care Management Enrollment & Eligibility
Our chronic care management solutions begin with accurate patient enrollment and eligibility checks. We manage Medicare eligibility validation and enrollment tracking using proven chronic care management enrollment solutions. This ensures only qualified patients are enrolled and billed. By setting up CCM programs correctly from day one, we help practices avoid audits, reduce billing errors, and build a stable, compliant CCM foundation.
AI-Powered Compliant CCM Coding & Monthly Billing
We provide dependable chronic care management billing solutions that follow CMS rules for time-based CCM services. Our team validates monthly time logs, confirms CPT thresholds, and reviews documentation before billing. This ensures claims are accurate, compliant, and submitted on time. With consistent and correct billing, practices can rely on predictable monthly revenue while staying fully aligned with Medicare CCM requirements.

Automated Denial Prevention & Revenue Protection
Our solutions use AI-powered pre-billing checks to catch issues before claims are submitted. We review eligibility, consent status, time logs, and medical necessity upfront. This proactive process reduces denials, prevents payment delays, and protects monthly CCM revenue. By fixing problems early, we help practices maintain steady cash flow and avoid repeated billing issues.
Who We Serve

Solo Primary Care Practitioners

Multi-Provider Primary Care

Hospital-Based Primary Care

Solo Primary Care Practitioners

Multi-Provider Primary Care

Hospital-Based Primary Care
Losing monthly CCM revenue for missed time tracking or errors?
We Are Certified by














